What is Gastroschisis?
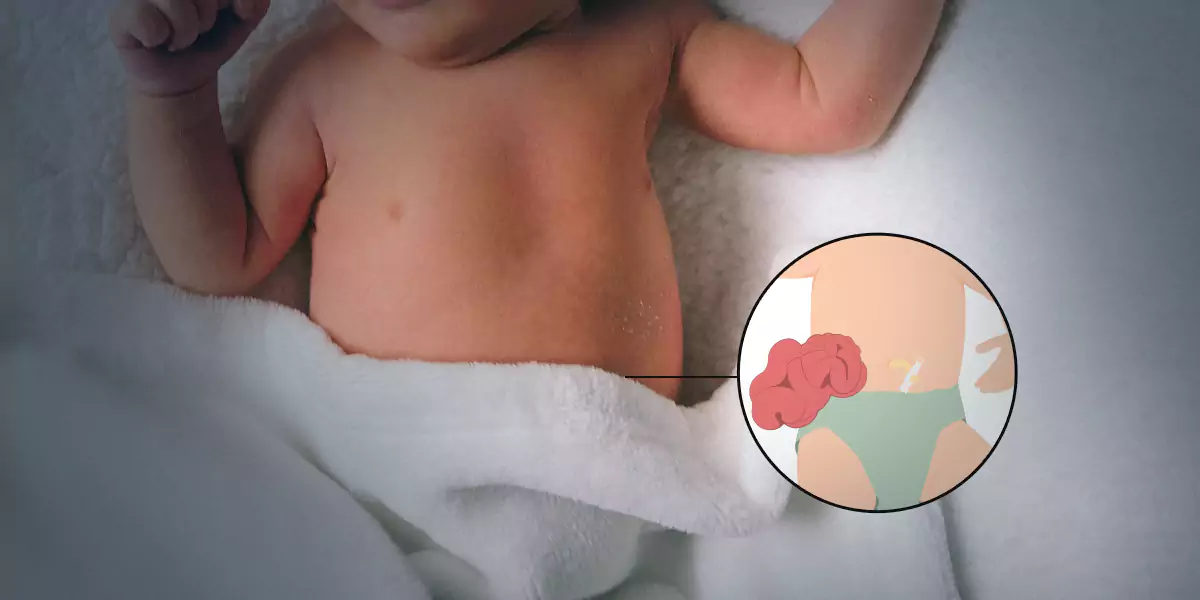
Gastroschisis is a birth defect in which your baby’s intestines (large or small intestines stomach,) remain outside their body from a 2 to 5-centimetre hole near their belly button during fetal development. Gastroschisis occurs during early pregnancy when your baby’s abdominal wall is not formed correctly, which leaves an opening for their organs to exit. The organs of the baby float in amniotic fluid inside your uterus, causing swelling and irritation. Surgery is needed to put your baby’s organs inside their body.
What are the Types of Gastroschisis?
Gastroschisis is mainly classified as simple or complicated. This depends on how inflamed the organs and/or bowel have moved through the opening.
With simple gastroschisis, only the bowel remains outside of the abdominal opening.
With complicated gastroschisis, one or more of the following happens:
– The bowel outside of the baby’s body is immensely damaged, for example; a part of the tissue dies, or the bowel becomes tangled or twisted.
– Intestinal atresia, in which a portion of the baby’s bowel is not completely formed, or the intestine gets blocked.
– Other organs, like the liver or stomach or liver, also protrude out of the opening.
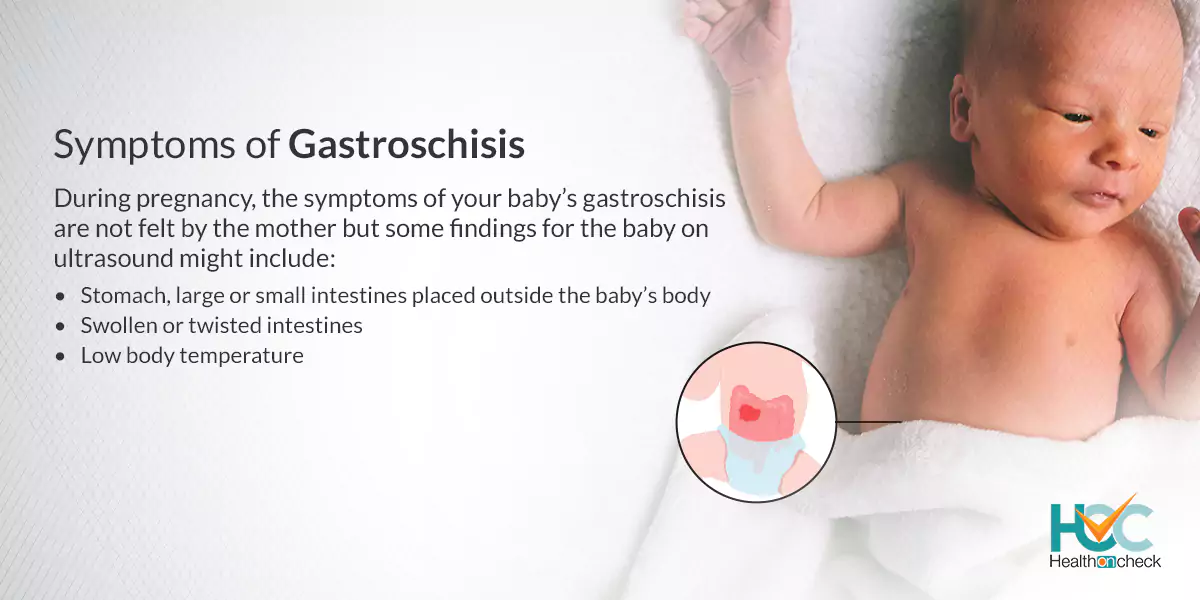
What are the Symptoms of Gastroschisis?
During pregnancy, the symptoms of your baby’s gastroschisis are not felt by the mother but some findings for the baby on ultrasound might include:
– Stomach, large or small intestines placed outside the baby’s body.
– Swollen or twisted intestines.
– Low body temperature.
What are the Causes of Gastroschisis?
The exact cause of gastroschisis is not yet known but it does not seem to be inherited. If you had one baby with gastroschisis that does not make it more necessary that you would have another baby with it. Gastroschisis usually occurs when your baby’s abdominal wall is not completely formed during foetal development in the womb. If you are planning to become pregnant, you should discuss with your doctor the ways to avert birth defects.
What are the Risk Factors of Gastroschisis?
The risk factors of gastroschisis usually include:
– Younger age
Teenage mothers have more chances of having a baby with gastroschisis than older mothers.
– Alcohol and tobacco
Women who smoked or consumed alcohol before or during early pregnancy have an increased risk of having a baby with gastroschisis.
– Genitourinary infections
Women who had genitourinary infection before or after three months of being pregnant have more chances to have a baby with gastroschisis as compared to women who had genitourinary infection during the second or third trimester of pregnancy
What are the Complications of Gastroschisis?
The complications of genitourinary might include sepsis, prolonged ileus, related intestinal atresias, wound infection, malabsorption, and necrotizing enterocolitis.
Babies with gastroschisis might be born prematurely or born small because of slow growth in the womb before birth. The complications of babies with gastroschisis might include:
– Breathing problems and heart problems
If your baby is born with gastroschisis then they might require a breathing tube and breathing machine for some days or weeks after surgery.
– Digestion and feeding problems
A baby born with gastroschisis might have an intestinal blockage or scar tissue that affects digestion. An intestinal blockage When food or stool is not moving through the intestines, an intestinal blockage occurs. Some organs might get damaged when your baby’s doctor squeezes them through the hole in the belly. It can reduce blood flow to the kidneys and intestines and cause digestion problems in your baby after birth.
– Infections
Necrotizing enterocolitis (also called NEC) develops in nearly one-third of the babies with gastroschisis. NEC occurs when the tissue of the intestine gets damaged because of which the tissue dies. In some instances, a hole might form in the intestine and if it occurs, the bacteria and waste from inside your baby’s intestine flow into the blood or the abdominal cavity and cause infections.
– Short bowel syndrome
In rare instances, some babies have missed parts in their intestines, preventing your baby from absorbing nutrients from food.
Also, complications might occur in your baby after gastroschisis surgery which may include:
– Infection at the surgical site.
– Problems in eating.
How Gastroschisis is Diagnosed?
The diagnosis of gastroschisis might occur either during pregnancy or after the baby is born. Diagnosis generally happens around 18 to 20 weeks of pregnancy with routine prenatal tests checking for birth defects in your baby. These tests routine prenatal tests include:
– Ultrasound
It’s an imaging test where sound waves are used to see detailed images of soft tissues inside your body.
– Blood screening
A blood test helps to measure substances in your blood, such as alpha-fetoprotein, and if it’s found higher than normal levels between 18 and 22 weeks, then it can be a sign of gastroschisis.
– Magnetic resonance imaging (MRI)
It’s an imaging test where a detailed picture of the inside of your body and the baby is taken which helps in diagnosing birth defects including gastroschisis.
What are the Treatment Options Available for Gastroschisis?
Even though a gastroschisis diagnosis usually happens during pregnancy, treatment can’t begin until after your baby is born.
Surgery is needed to place your baby’s organs back inside their body along with repairing the hole beside their belly button to stop their organs from returning outside of their body.
Based on the severity of the condition and how many organs are there outside the baby’s body, two types of surgery are available to relocate your baby’s organs along with repairing their abdominal wall:
– Primary repair
Here, your baby will receive surgery right after the baby is born to place the organs back into their body along with repairing the hole in their abdomen.
– Staged repair
For instance, gastroschisis is more complicated, the surgery will be done slowly in stages. A staged repair is most effective when the baby isn’t healthy enough for surgery, or if the abdomen isn’t large enough to hold all of the organs.
Your baby’s surgeon will put their exposed organs in a plastic pouch known as a silo to prevent damage, infection, and dehydration from the time your baby is born to the time of their surgery to repair gastroschisis.
Additional surgery might be required to repair your baby’s abdomen muscles or intestines may be necessary after the initial surgery.
Living with Gastroschisis
It may be stressful and scary for you to see your baby born with their organs outside of their body, but the prognosis after surgery for replacing their organs back into their body is quite positive. Your doctor will be available there to answer any query you might have about your baby’s condition and to guide you through the surgery and recovery process of your baby.
Whom to Consult?
If your baby is diagnosed with Gastroschisis, then it’s best to deliver your baby to a hospital with specialists who can take proper care of your baby’s condition in a neonatal intensive care unit (NICU). Babies with gastroschisis can be safely born vaginally or through caesarean section (c-section). Your doctor will guide you to determine the best delivery method for your baby.